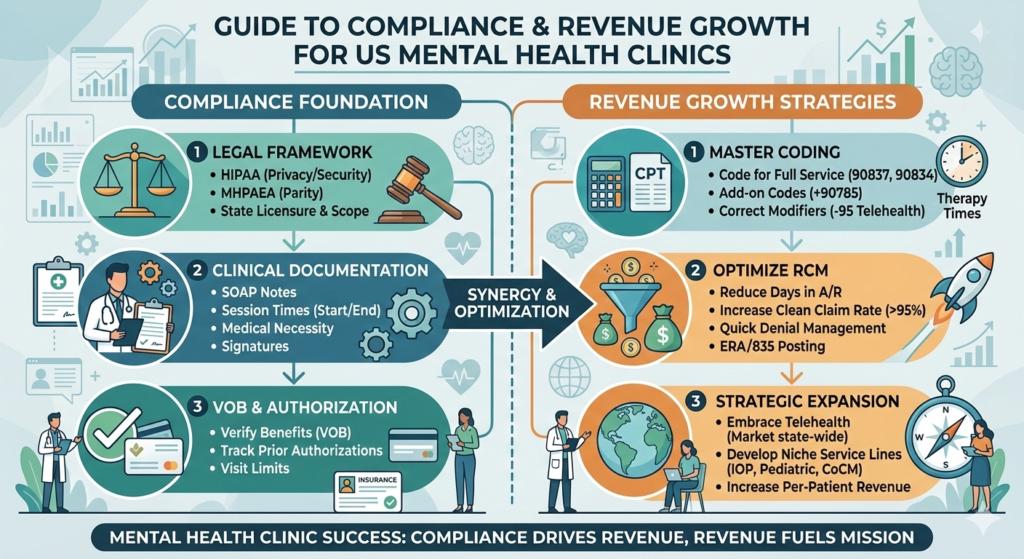
The demand for behavioral health treatment in the United States continues to grow. With rising awareness of anxiety, depression, trauma-related disorders, substance use conditions, and telehealth-based therapy, providers are seeing more patients than ever before. However, behind every therapy session or psychiatric evaluation lies a complex administrative process that determines whether the provider gets paid accurately and on time.
Behavioral and mental health billing services are not just about submitting claims. They involve compliance, documentation accuracy, payer rules, coding precision, and constant follow-up. For many clinics and private practices, billing has become one of the biggest operational challenges.
This guide explains how mental health billing works, common pain points, why outsourcing is becoming popular, and how to choose the right support partner in the USA.
Why Behavioral and Mental Health Billing Is Different
Billing for mental health providers is significantly different from general medical billing. The codes, documentation standards, and reimbursement rules are highly specific. For example, psychotherapy sessions are time-based, psychiatric evaluations require detailed notes, and telehealth billing has its own modifiers and payer variations.
Behavioral and mental health billing services must handle:
-
Time-based CPT coding for psychotherapy
-
Add-on codes for crisis therapy
-
Telehealth modifiers and POS codes
-
Prior authorizations for ongoing sessions
-
Coordination with Medicaid, Medicare, and commercial payers
Even small documentation errors can lead to denials. That is why many clinics now look for a mental health billing services company that understands payer psychology and behavioral health regulations in depth.
Core Components of Mental Health Billing
A structured approach to mental health billing typically includes:
Patient Eligibility Verification
Insurance coverage for therapy often varies by session limits and diagnosis. Verifying benefits before appointments reduces claim denials.
Accurate Coding
Coding and billing for mental health services requires precise CPT and ICD-10 pairing. Improper coding may result in reduced reimbursement or compliance risks.
Authorization Management
Many payers require prior authorization after a certain number of sessions. Tracking approvals is essential.
Claims Submission
Electronic claim submission must include correct modifiers, place of service codes, and documentation references.
Denial Management
Appeals require strong clinical documentation and knowledge of payer-specific rules.
Payment Posting and Reporting
Tracking reimbursements ensures transparency in revenue cycle management.
When handled correctly, mental health billing solutions can improve cash flow and reduce administrative stress.
Common Challenges in Billing for Mental Health Services
Providers across the USA face recurring billing challenges:
-
Frequent claim denials due to incomplete documentation
-
Incorrect time-based coding
-
Telehealth compliance confusion
-
Delays in billing Medicare for mental health services
-
Credentialing delays affecting reimbursement
Billing for mental health therapists is especially complex for solo practitioners who juggle clinical work and administration. In such cases, outsourced billing for mental health becomes a strategic decision rather than a cost.
In-House vs Outsourcing Mental Health Billing
Many practices initially manage billing internally. Over time, they realize that administrative overhead affects patient care and revenue.
In-House Billing
-
Requires trained staff
-
Ongoing training on payer updates
-
Salary, software, and compliance costs
-
Risk of staff turnover
Outsourcing Mental Health Billing
-
Access to specialized billing teams
-
Lower operational overhead
-
Improved denial management
-
Scalable solutions for growing practices
Outsourcing mental health billing and coding allows providers to focus on patient care while experienced professionals manage the revenue cycle.
What to Look for in a Mental Health Billing Company
Not all billing companies for mental health are equal. Choosing the right partner requires careful evaluation.
A reliable mental health billing company should provide:
-
Experience with psychotherapy and psychiatry billing
-
Expertise in billing Medicare for mental health services
-
Credentialing support
-
Transparent reporting
-
HIPAA compliance
Many providers search for the best mental health billing services company, but the real value lies in experience, communication, and proven results rather than marketing claims.
Some practices prefer a top mental health billing company with national experience, while smaller clinics may look for a specialized mental health billing specialist companies that understand local payer policies.
Cost is also a factor. While some providers consider hiring a cheap outsource mental health billing company, lower cost should not compromise compliance or accuracy. Billing errors can be far more expensive than service fees.
Mental Health Billing and Credentialing Services
Credentialing is a critical but often overlooked part of behavioral health operations. Without proper enrollment with payers, claims cannot be reimbursed.
Mental health billing and credentialing services ensure:
-
Enrollment with Medicare and Medicaid
-
Commercial insurance registration
-
CAQH profile maintenance
-
Re-credentialing updates
Credentialing delays are one of the biggest reasons new practices struggle financially during their first year. Partnering with a mental health billing services company that offers credentialing support creates smoother revenue flow.
Medical Billing for Mental Health: Compliance Matters
Compliance is a central part of mental health medical billing. Behavioral health documentation must support medical necessity. Audits can happen at any time, especially with government payers.
Billing for mental health must align with:
-
Federal mental health parity laws
-
CMS guidelines
-
State Medicaid policies
-
Telehealth billing regulations
An experienced mental health billing company monitors policy updates and adjusts coding practices accordingly.
Telehealth and Behavioral Health Billing Trends
Since telehealth expansion in the United States, behavioral and mental health billing services have adapted to virtual care models.
Key telehealth billing considerations include:
-
Correct use of telehealth modifiers
-
Audio-only session compliance
-
Cross-state licensing issues
-
Insurance parity policies
Practices that fail to adjust telehealth billing protocols often experience reimbursement delays. This is where the best outsource mental health billing and coding services provide strategic advantage.
Revenue Cycle Optimization for Mental Health Clinics
Efficient billing services for mental health clinics directly impact revenue stability.
Optimized billing processes lead to:
-
Faster claim turnaround
-
Reduced aging accounts receivable
-
Improved clean claim rate
-
Higher reimbursement accuracy
Behavioral and mental health billing services are most effective when integrated into a broader revenue cycle management strategy.
For growing group practices, billing mental health services efficiently allows expansion without increasing administrative burden.
Why Many Providers Choose Outsourced Billing
Outsourced billing for mental health has grown rapidly because of increasing regulatory complexity. Practices want predictability in collections.
Benefits often include:
-
Dedicated account managers
-
Proactive denial follow-up
-
Monthly performance reports
-
Compliance monitoring
The best mental health billing company operates as an extension of the provider’s team, not just a vendor.
When evaluating billing services for mental health, ask about performance metrics such as:
-
Clean claim rate
-
Average days in AR
-
Denial percentage
-
First-pass resolution rate
These indicators reflect operational efficiency better than promotional language.
Future of Behavioral and Mental Health Billing Services in USA
Mental healthcare demand continues to expand across the United States. With insurance reforms and digital health adoption, billing structures will keep evolving.
We are seeing:
-
Increased payer scrutiny
-
Integration of AI-based billing audits
-
Expansion of value-based care models
-
Greater documentation requirements
Practices that invest in professional mental health billing solutions position themselves for long-term sustainability.
Partnering for Sustainable Growth
Reliable billing support ensures that providers focus on therapy, assessments, and patient relationships rather than administrative confusion.
Organizations like 247 medical billing services provide comprehensive medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services tailored to healthcare providers, including behavioral health practices. When aligned with experienced billing teams, mental health clinics can achieve consistent reimbursements while maintaining compliance and operational clarity.
Conclusion
Behavioral and mental health billing services are essential for financial stability in today’s complex healthcare environment. From eligibility verification to denial management and credentialing, every step impacts reimbursement outcomes.
Whether you operate a solo therapy practice or a multi-provider clinic, choosing the right mental health billing services company can improve cash flow, reduce stress, and strengthen compliance. As regulations evolve in the USA, professional billing support is no longer optional but a strategic necessity.
Frequently Asked Questions
What are behavioral and mental health billing services?
Behavioral and mental health billing services manage insurance claims, coding, authorizations, and reimbursement processes specifically for psychotherapy, psychiatry, and counseling practices.
Why is billing for mental health different from general medical billing?
It involves time-based CPT codes, therapy session limits, prior authorizations, and unique documentation standards that differ from standard medical procedures.
Is outsourcing mental health billing a good idea for small practices?
Yes, outsourcing mental health billing and coding can reduce administrative workload, improve claim accuracy, and enhance collections, especially for solo providers.
How do billing companies for mental health improve revenue?
They reduce denials, ensure correct coding, manage authorizations, and monitor payer updates to maintain consistent reimbursement flow.
What should I look for in a mental health billing services company?
Look for experience in mental health medical billing, transparent reporting, credentialing expertise, Medicare billing knowledge, and strong denial management processes.
Can mental health billing services handle Medicare claims?
Yes, experienced teams manage billing Medicare for mental health services, including compliance with CMS documentation and coding guidelines.
Do billing services for mental health clinics include credentialing?
Many providers offer mental health billing and credentialing services to ensure smooth enrollment and uninterrupted claim submission.