Behavioral health practices in Virginia are facing a unique mix of rising patient demand, evolving payer rules, and increasing administrative complexity. From mental health clinics to substance use treatment centers, providers are expected to deliver quality care while maintaining accurate and compliant billing operations. This is where outsourcing behavioral health billing virginia becomes a strategic decision rather than just an operational choice.
Outsourcing is no longer limited to large healthcare systems. Small and mid-sized behavioral health providers are increasingly turning to specialized billing partners to streamline revenue cycle processes, reduce denials, and improve financial stability.
Why Behavioral Health Billing Is More Complex Than Ever
Behavioral health billing differs significantly from general medical billing due to several factors:
-
Frequent changes in CPT and ICD coding for mental health services
-
Strict documentation requirements for therapy sessions and treatment plans
-
Payer-specific policies for telehealth and substance abuse treatment
-
Pre-authorization and eligibility verification complexities
-
High denial rates due to coding and compliance errors
These challenges make it difficult for in-house teams to maintain efficiency, especially when resources are limited.
Key Benefits of Outsourcing Behavioral Health Billing in Virginia
Outsourcing behavioral health billing virginia provides measurable advantages that directly impact a practice’s financial health and operational efficiency.
Improved Revenue Cycle Performance
Specialized billing companies ensure accurate claim submissions, faster reimbursements, and reduced claim rejections.
Access to Industry Expertise
Experienced billing professionals stay updated with state and federal regulations, including Medicaid and commercial payer policies in Virginia.
Reduced Administrative Burden
Outsourcing allows clinicians and staff to focus more on patient care instead of handling billing complexities.
Better Compliance and Risk Management
Professional billing services ensure adherence to HIPAA regulations and payer guidelines, minimizing audit risks.
Scalability for Growing Practices
As your practice expands, outsourced billing solutions can easily scale without the need for additional in-house hiring.
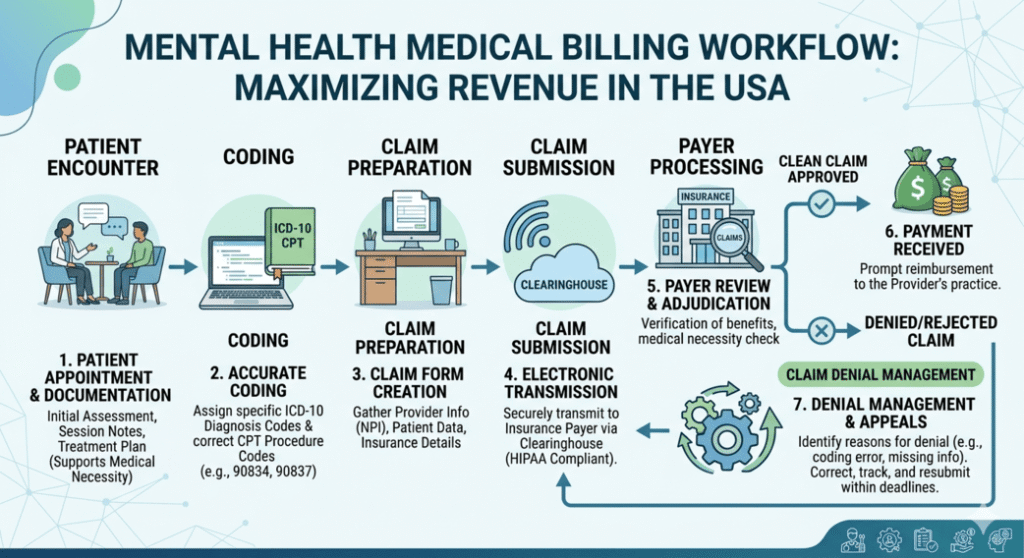
How Outsourcing Works in Behavioral Health Billing
The outsourcing process typically follows a structured workflow:
Patient Registration and Eligibility Verification
Ensuring accurate patient data and insurance coverage before services are provided.
Coding and Charge Entry
Certified coders assign appropriate CPT and ICD codes based on documentation.
Claim Submission
Clean claims are submitted electronically to insurance payers.
Payment Posting
Payments are accurately recorded, and discrepancies are flagged.
Denial Management and Appeals
Rejected claims are analyzed and resubmitted with corrections.
Accounts Receivable Follow-Up
Outstanding claims are tracked and resolved promptly.
This structured approach ensures consistency and efficiency across the revenue cycle.
Why Virginia Providers Are Choosing Outsourcing
Healthcare providers in Virginia are increasingly recognizing the value of outsourcing due to:
-
Growing mental health awareness and patient volume
-
Expansion of telehealth services
-
Complex Medicaid billing requirements
-
Shortage of skilled billing professionals
By outsourcing behavioral health billing virginia, practices can maintain financial stability while adapting to these changes.
Comparing Billing Trends Across States
While Virginia has its own regulatory environment, outsourcing trends are consistent across the United States. For example:
Providers offering outsourcing behavioral health billing ohio and outsourcing community behavioral health billing ohio are focusing on improving Medicaid reimbursements and compliance.
Organizations using outsourcing behavioral health billing services connecticut and professional behavioral health billing company connecticut emphasize precision in documentation and payer communication.
In regions like outsourcing behavioral health billing services delaware and community behavioral health billing services company delaware, smaller practices rely heavily on outsourcing to manage limited resources.
States such as outsourcing behavioral health billing services florida and outsourcing behavioral health billing texas are seeing rapid growth due to large patient populations and diverse payer networks.
These trends highlight the importance of specialized billing support regardless of location.
Choosing the Right Behavioral Health Billing Partner
Selecting the right billing partner is critical to achieving desired outcomes. Here are key factors to consider:
Experience in Behavioral Health
Look for a company with proven expertise in mental health and substance abuse billing.
Technology and Automation
Advanced billing software ensures accuracy, transparency, and real-time reporting.
Compliance Knowledge
The partner should be well-versed in HIPAA, Medicare, Medicaid, and commercial payer requirements.
Transparent Pricing
Clear pricing models help avoid hidden costs and ensure better financial planning.
Client Support and Communication
Reliable support ensures quick resolution of issues and consistent performance.
Many providers compare options like behavioral health billing company california, behavioral health billing services in california, and behavioral health billing company georgia to identify best practices and service standards.
Common Challenges Solved by Outsourcing
Outsourcing addresses several pain points faced by behavioral health providers:
High Claim Denial Rates
Professional billing teams identify root causes and implement corrective measures.
Delayed Payments
Efficient claim submission and follow-up reduce payment cycles.
Coding Errors
Certified coders ensure accurate coding aligned with documentation.
Staff Turnover
Outsourcing eliminates dependency on in-house billing staff.
Compliance Risks
Regular audits and updates ensure adherence to regulations.
Practices offering behavioral health billing columbus and behavioral health billing columbus ohio have particularly benefited from outsourcing due to improved efficiency and reduced administrative stress.
Expanding Beyond Virginia: A Nationwide Perspective
Behavioral health billing outsourcing is not limited to Virginia. Providers across the country are leveraging these services:
Organizations using behavioral health billing services north carolina and best behavioral health billing company south carolina focus on improving payer relationships and reimbursement rates.
Providers working with professional behavioral health billing company new hampshire and professional behavioral health billing company rhode island prioritize compliance and audit readiness.
Facilities offering behavioral health billing services rhode island and behavioral health medical billing utah emphasize accuracy in coding and documentation.
These examples demonstrate how outsourcing has become a standard practice in modern healthcare revenue management.
The Future of Behavioral Health Billing
The future of behavioral health billing will be shaped by:
Increased Use of Telehealth
Billing systems must adapt to virtual care models and evolving reimbursement policies.
Integration of AI and Automation
Automation will reduce manual errors and improve efficiency.
Value-Based Care Models
Providers will need to focus on outcomes rather than volume.
Stricter Compliance Requirements
Regulatory changes will require continuous updates and monitoring.
Outsourcing partners play a crucial role in helping practices navigate these changes effectively.
How 247 Medical Billing Services Supports Behavioral Health Providers
For practices seeking reliable support, 247 medical billing services offers comprehensive solutions tailored to behavioral health providers. Their services include medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services.
By combining industry expertise with advanced technology, they help practices optimize revenue, reduce denials, and maintain compliance.
Conclusion
Outsourcing behavioral health billing virginia is more than a cost-saving strategy. It is a pathway to improved efficiency, compliance, and financial growth. As the demand for behavioral health services continues to rise, providers must adopt smarter operational strategies to stay competitive.
With the right billing partner, practices can focus on delivering quality care while ensuring a stable and optimized revenue cycle.
Frequently Asked Questions
What is behavioral health billing outsourcing
Behavioral health billing outsourcing involves delegating billing tasks such as coding, claim submission, and payment follow-up to a specialized third-party provider.
Why should Virginia providers outsource billing
Outsourcing helps reduce administrative workload, improve claim accuracy, and ensure compliance with complex billing regulations.
Is outsourcing cost-effective for small practices
Yes, outsourcing eliminates the need for in-house billing staff and reduces errors, making it a cost-effective solution for small and mid-sized practices.
How does outsourcing reduce claim denials
Experienced billing teams use accurate coding, proper documentation, and payer-specific guidelines to minimize errors and rejections.
Can outsourcing handle multiple insurance providers
Yes, professional billing companies are equipped to manage billing for Medicare, Medicaid, and commercial insurance plans.
What should I look for in a billing partner
Key factors include experience in behavioral health, compliance expertise, advanced technology, transparent pricing, and reliable support.