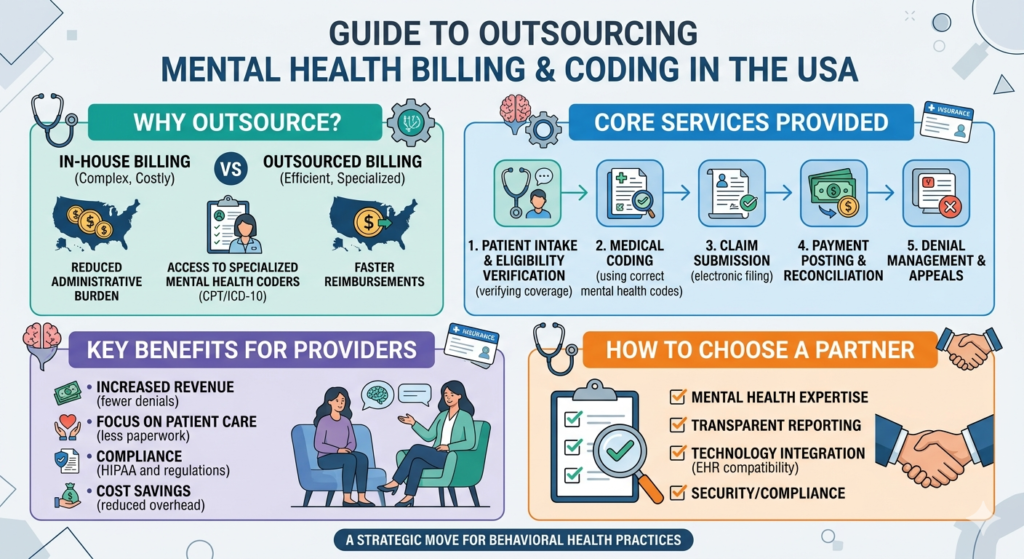
Mental health practices in New York operate in one of the most complex healthcare environments in the United States. From strict payer requirements to evolving telehealth regulations, billing is no longer just administrative work—it directly impacts revenue, compliance, and patient satisfaction. Choosing the right mental health billing services New York providers can rely on is essential for sustainable growth.
This guide explores how billing works in mental health, why outsourcing is becoming the norm, and what to look for when selecting a trusted partner.
Why Mental Health Billing Requires Specialized Expertise
Mental health billing is not the same as general medical billing. It involves unique coding systems, session-based documentation, and strict payer guidelines.
Key challenges include:
-
Complex CPT and ICD coding
Therapy sessions, psychiatric evaluations, and medication management require precise coding to avoid denials. -
Frequent claim denials
Errors in documentation or authorization often lead to rejected claims. -
Insurance variability
Each payer has different rules for mental health coverage and reimbursement. -
Compliance requirements
HIPAA, state-specific laws, and parity regulations must be followed closely.
Because of these challenges, many providers are shifting toward outsourcing mental health billing and coding services to improve accuracy and reduce administrative burden.
What Do Mental Health Billing Services Include?
A reliable billing partner offers end-to-end revenue cycle support tailored to behavioral health practices.
Core services typically include:
-
Patient eligibility and benefits verification
Ensuring coverage before services are rendered. -
Accurate coding and charge entry
Minimizing claim errors and maximizing reimbursement. -
Claims submission and tracking
Timely filing and proactive follow-up. -
Denial management and appeals
Identifying root causes and recovering lost revenue. -
Payment posting and reporting
Transparent financial insights for better decision-making. -
Compliance monitoring
Keeping your practice aligned with regulatory standards.
When selecting billing services for mental health providers New York, these capabilities should be standard—not optional.
Benefits of Outsourcing Mental Health Billing in New York
Outsourcing has become a strategic move rather than just a cost-saving tactic.
Here’s why:
-
Improved revenue cycle performance
Faster claims processing and reduced denials lead to consistent cash flow. -
Cost efficiency
Compared to hiring an in-house team, outsourcing reduces overhead expenses. -
Access to experienced professionals
Specialists stay updated on payer policies and coding changes. -
More time for patient care
Providers can focus on therapy instead of paperwork. -
Scalability
Easily manage growth without expanding internal staff.
Many practices searching for mental health billing services near me ultimately choose outsourcing for these advantages.
Choosing the Best Mental Health Billing Services Company New York
Not all billing providers deliver the same level of service. Selecting the right partner requires careful evaluation.
Consider these factors:
-
Industry experience
Look for companies specializing in behavioral health, not general billing. -
Technology and automation
Advanced systems improve accuracy and efficiency. -
Transparent reporting
Real-time dashboards and financial insights are essential. -
Compliance knowledge
Familiarity with New York regulations is critical. -
Client support
Dedicated account managers ensure smooth communication.
A best mental health billing company New York will not only process claims but also act as a strategic partner in your growth.
How Mental Health Billing in New York Compares Nationwide
While New York has its own complexities, mental health billing practices vary across states. Understanding these differences helps providers benchmark performance.
For example:
-
Providers exploring mental health billing services Pennsylvania often encounter different payer policies compared to New York.
-
In regions like mental health billing Ohio or mental health billing Dayton Ohio, reimbursement rates and payer mix may differ significantly.
-
Cities such as mental health billing Cincinnati Ohio highlight regional variations in claim approval timelines.
-
Practices evaluating mental health billing Massachusetts or mental health billing services Florida face unique compliance and documentation requirements.
-
In the South, demand for affordable options has led to searches for cheap mental health billing company South Carolina and cheap mental health billing company Virginia.
-
States like California remain highly competitive, with numerous mental health billing companies in California offering specialized services, including mental health billing services California and mental health billing services in California.
-
Providers in Texas often seek scalable solutions such as billing services for mental health providers Texas or even a top mental health billing company Texas for large practices.
-
Similarly, Florida practices rely on options like billing services for mental health providers Florida, mental health billing agency Florida, and florida mental health medical billing outsourcing services.
This nationwide perspective shows why choosing a local expert for mental health billing services in New York is crucial—state-specific knowledge makes a difference.
Common Mistakes in Mental Health Billing
Even experienced providers can lose revenue due to avoidable errors.
Watch out for:
-
Incorrect coding
Using outdated or mismatched CPT codes. -
Incomplete documentation
Missing session notes or medical necessity details. -
Failure to verify insurance
Leads to denied or delayed claims. -
Late claim submission
Missing payer deadlines can result in lost revenue. -
Ignoring denial patterns
Without analysis, the same issues repeat.
A professional mental health billing services company Florida or New York-based provider will actively monitor and resolve these issues.
The Role of Technology in Mental Health Billing
Modern billing services rely heavily on technology to improve outcomes.
Key innovations include:
-
AI-driven claim scrubbing
Detects errors before submission. -
Automated eligibility checks
Reduces front-end mistakes. -
Integrated EHR systems
Ensures seamless documentation and billing flow. -
Real-time analytics
Provides insights into revenue trends and performance.
Whether you’re working with a mental health billing service in California or New York, technology is a major differentiator.
How to Get Started with Mental Health Billing Services
Transitioning to a new billing partner doesn’t have to be complicated.
Steps include:
-
Evaluate your current billing performance
Identify gaps and revenue leakage. -
Define your goals
Faster payments, reduced denials, or improved compliance. -
Research providers
Compare experience, pricing, and services. -
Request a billing audit
Understand potential improvements. -
Plan a smooth transition
Ensure minimal disruption to operations.
Many providers looking for cheap mental health billing company Texas or cheap mental health billing company north carolina realize that value matters more than just price.
Why Location-Specific Expertise Matters in New York
New York has strict healthcare regulations and diverse payer networks. Billing services for mental health providers New York must understand:
-
Medicaid and Medicare nuances
-
Commercial insurance policies
-
Telehealth billing guidelines
-
State compliance requirements
A generic billing company may not provide the same level of precision as a specialized local provider.
Conclusion
Mental health billing is a critical component of a successful practice. With increasing administrative complexity, outsourcing is no longer optional—it’s a strategic necessity.
Choosing the right mental health billing services New York partner can improve revenue, reduce stress, and allow providers to focus on what truly matters: patient care.
For practices aiming to scale efficiently, working with a trusted partner that offers comprehensive support—from coding to revenue cycle management—can make all the difference. Companies like 247 medical billing services bring together medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services to deliver a complete solution tailored for mental health providers.
FAQs
1. What are mental health billing services?
Mental health billing services handle coding, claim submission, and reimbursement processes specifically for behavioral health providers.
2. Why should I outsource mental health billing?
Outsourcing improves accuracy, reduces denials, and allows providers to focus more on patient care.
3. How do I choose the best mental health billing company in New York?
Look for experience, transparency, compliance expertise, and strong client support.
4. Are mental health billing services expensive?
Costs vary, but outsourcing is often more cost-effective than maintaining an in-house team.
5. Can billing services help reduce claim denials?
Yes, experienced billing companies identify errors early and manage appeals effectively.
6. Do billing services handle insurance verification?
Most providers include eligibility and benefits verification as part of their services.
7. Is mental health billing different from general medical billing?
Yes, it involves unique codes, session-based billing, and stricter documentation requirements.
8. How quickly can I see results after outsourcing billing?
Most practices notice improvements in revenue and claim approval rates within a few months.